A thoracic aortic aneurysm (TAA) is an enlargement in the upper part of the aorta, the major blood vessel that routes blood to the body. Thoracic aortic aneurysms can cause aortic dissection (splitting of the aortic wall) and aortic rupture, leading to life-threatening internal bleeding. The fist two figures in the illustration below show two types of thoracic aortic aneurysm, an ascending thoracic aneurysm and a descending aortic aneurysm. For more information on the third illustration of an abdominal aortic aneurysm below, see the Abdominal Aortic Aneurysm page.
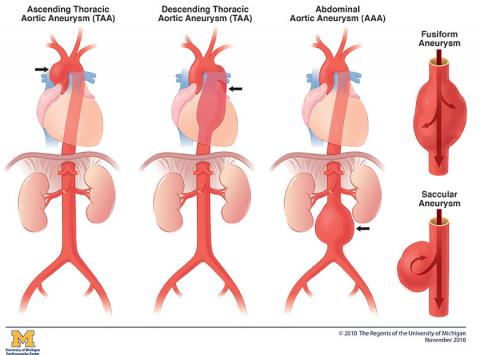
The above Illustration shows three types of aneurysm and the two aneurysm shapes. The three types of aneurysm are Ascending Thoracic aortic Aneurysm (TAA), Descending Thoracic Aortic Aneurysm (TAA), and Abdominal Aortic Aneurysm (AAA). The Fusiform Aneurysm and Saccular Aneurysm show the two types of aneurysm shapes.
Thoracic aortic aneurysms, even those that are large, frequently do not cause symptoms. Some individuals, however, may experience symptoms such as:
- Pain in the chest area
- Back pain
- Coughing or hoarseness
- Shortness of breath/difficulty breathing
An aneurysm can appear anywhere in the aorta, including:
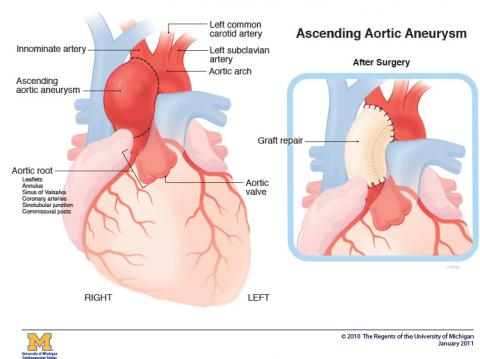
- Aortic root, the area where the aorta exits the heart and includes the openings to the coronary arteries
- Ascending aorta, which emerges from the top of the aortic root
- Aortic arch, the part of the aorta that arches and turns downward before it becomes the descending aorta
- Descending aorta, which branches into the thoracic and abdominal aorta. A descending aortic aneurysm that extends to the abdomen is a thoracoabdominal aneurysm.
- Abdominal aorta, which is located below the diaphragm
Risk Factors
Risk factors for a thoracic aortic aneurysm include:
- Genetic variants (Marfan, Loeys-Dietz and Ehlers-Danlos syndromes, familial thoracic aortic aneurysm, bicuspid aortic valve)
- High blood pressure (hypertension)
- Age
- Smoking
Diagnosis
Often, a thoracic aneurysm is not diagnosed until a rupture occurs. If your healthcare provider believes you may have a thoracic aortic aneurysm, the following tests may be given:
- Chest X-ray
- Computed tomography (CT) scan
- Magnetic resonance imaging (MRI)
- Echocardiography (ultrasound of the heart)
- Abdominal ultrasound
- Angiography (X-ray of the blood vessels)
Treatment
Treatment options for ascending, arch, descending and root aortic aneurysms may include:
- Regular screenings to monitor the size and growth of the aneurysm to determine if treatment — including surgery — is necessary
- Surgery, including both open and endovascular options
- Lifestyle changes such as smoking cessation, controlling diabetes and a low-fat diet to reduce cholesterol levels. These changes may help keep the aneurysm from growing.
- Medication to help reduce high blood pressure and cholesterol levels
Surgical and Endovascular Treatment
Thoracic aortic aneurysms sometimes require complex open-heart surgery, including the use of hypothermic circulatory arrest (HCA), a technique that uses very cold body temperatures to temporarily stop blood flow to the area of the aorta being operated on. A valve replacement may be necessary, depending on the location and extent of the rupture. Surgery may involve replacing the weakened area of the aorta with a graft or artificial material.
A valve-sparing aortic root replacement may also be an option for root aneurysm patients with a normal aortic valve. This procedure replaces the aortic root while preserving the patient’s aortic valve.
For many patients with descending thoracic aortic aneurysms, an endovascular treatment known as thoracic endovascular aortic repair (TEVAR) is an alternative to conventional open-heart surgery. This minimally invasive endovascular option for some patients who are not optimal candidates for traditional open repair can shorten hospital stays and reduce recovery periods.
For high-risk patients with arch aneurysms, we offer a less invasive debranching option that bypasses arch vessels and eliminates the need for hypothermic circulatory arrest.
Similarly, patients with thoracoabdominal aneurysms (aneurysms that coexist in both the chest and the abdomen) may also be candidates for the debranching option, which eliminates the need for a large thoracoabdominal incision.
We are also one of a few centers that offers descending thoracic aortic repair and maintain very favorable outcomes despite the complexity of the procedure.
The University of Michigan Frankel Cardiovascular Center is an early pioneer in TEVAR. We have extensive experience successfully treating high-risk patients. Visit our TEVAR page for more information about this minimally invasive option.
The University of Michigan Health Comprehensive Aortic Program
The Comprehensive Aortic Program at the U-M Frankel Cardiovascular Center is the most experienced in the state, and one of the largest in the country. Our documented outcomes include some of the lowest mortality rates for even the most complex thoracic aortic reconstructions.
Research Brings New Treatment Options for Aortic Disease
We continue to discover innovative and improved treatment options for aortic diseases. The University of Michigan is home to the International Registry of Aortic Dissection and several research laboratories that are exploring the molecular etiologies of aortic diseases. Through patient participation and research, we are helping to advance the best treatment options for all types of aortic diseases.
Make an Appointment
To schedule an appointment to discuss an aortic aneurysm or any other cardiovascular condition, call us at 888-287-1082 or visit our Make a Cardiovascular Appointment page, where you may view other information about scheduling a cardiovascular appointment.