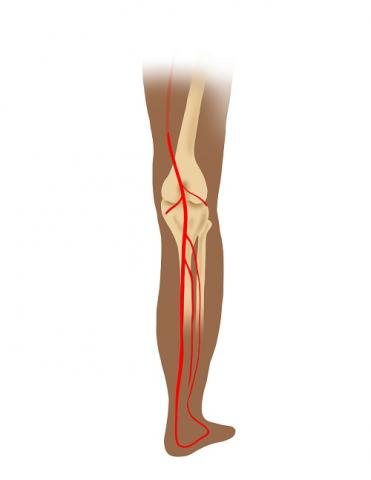
Popliteal artery entrapment syndrome (PAES) is a rare vascular condition that affects the legs. It occurs when the popliteal artery — the dominant source of blood supply to the leg below the knee — becomes compressed by a muscle, tendon or band behind the knee. This compression restricts blood flow to the lower leg and can cause damage to the artery over time.
PAES affects individuals under the age of 55, but is more commonly diagnosed in younger, highly active athletes whose calf muscles become enlarged due to exercise and training. Men are two times more likely than women to have the condition.
Symptoms of PAES
Patients with PAES typically experience an onset of symptoms associated with exercise, which may include:
- Aching pain (claudication), numbness or cramping in one or both calves during strenuous exercise (typically occurring within 5 or 10 minutes and subsiding when exercise stops)
- Swelling in the calf area
- Changes in skin color around the calf muscle
- Numbness, tingling and discoloration of the feet
- Pain in the lower leg and feet at rest (in patients with advanced PAES)
Diagnosis
The vascular surgery team at Michigan Medicine has extensive expertise in the diagnosis and treatment of PAES. The condition is often difficult to diagnose because it can mimic other conditions such as knee joint pain or other muscle-related problems.
Our experts diagnose PAES based on a patient’s medical history, a physical exam and non-invasive diagnostic testing. These tests may include:
- Ankle brachial index measurement with exercise to measure the blood pressure in the arms and legs before and after exercise.
- Duplex ultrasound, which uses sound waves to image the artery and measure blood flow.
- Computed tomographic angiography (CTA), which uses dye to identify areas around the knee with poor blood flow or narrowed arteries.
- Magnetic resonance angiography (MRA) to provide images of muscles, tendons and blood vessels.
- Angiogram with intravascular ultrasound (IVUS), which captures real-time images of blood flow while the leg and foot are maneuvered into various positions.
Treatment
If compression is detected and the popliteal artery remains healthy, surgery most often results in restoring normal blood flow to the leg. During this surgery, an incision is made behind the knee to access the popliteal artery, and the muscle, tendon or band causing the compression is relieved.
In more advanced cases, the compression may cause permanent change to the artery or complete blockage. For these patients, bypass surgery is performed using either a vein or synthetic graft to bypass the blocked section of the artery to create a new pathway for blood to reach the lower leg. The muscle, tendon or band responsible for the compression is also corrected.
Recovery for either surgery is 4-6 weeks, depending on the individual’s level of activity, with high-intensity athletes requiring the longest recovery period.
Michigan Medicine's Multidisciplinary Vascular Team
Michigan Medicine’s multidisciplinary vascular team includes vascular surgeons, nurse practitioners and sports medicine specialists with expertise in diagnosis and treatment of patients with popliteal artery entrapment syndrome. Michigan Medicine vascular surgeon Katherine Gallagher, M.D., is a foremost expert on the condition and has developed an algorithm for diagnosing patients. She also presents nationally on this topic. For more details on popliteal artery entrapment syndrome, refer to her publications:
- Campbell D, Andraska E, Rectenwald J, Gallagher KA: IVUS as a Novel Tool for the Diagnosis of Endofibrosis JVS-CIT 2(2): 59-61, 2016.
- Boniakowski A, Davis F, Campbell D, Khaja M, Gallagher KA: Intravascular ultrasound as a novel tool for the diagnosis and targeted treatment of functional popliteal artery entrapment syndrome. Journal of Vascular Surgery Cases and Innovative Techniques online: 74-78, 2017. 29349382.
Make an Appointment
To schedule an appointment to discuss your cardiovascular condition, call us at 888-287-1082, or visit our Make an Appointment page for more information about what to expect when you call us.